In short, the old way didn't work very well. If non-blood colloids were used, they would either clog the kidneys (hydroxyethyl starch) or incorporate themselves into newly formed clots, degrading the clot integrity ( gelofusine). Lungs would fill with oedema and become stiff oedematous gut would refuse to perform normal peristaltic work, and oedematous anastomotic sites would break down due to poor perfusion. The oedematous tissues would swell, limiting vascular access and creating compartment syndromes. 
Such unbalanced resuscitation strategies lead to depletion of coagulation factors and exacerbation of dilutional coagulopathy. Shoemaker at al, 1976) it seems the disadvantages of this approach were already clear. This carried on for some time, even though from the literature of the period (eg. The goal was to flog the patient with fluid boluses, with the goal being a normal arterial blood pressure. Then, when coags become abnormal, other blood products would be used. Historically, vast volumes of crystalloid would be funnelled into the patient in order to restore the circulating volume, with occasional units of packed cells thrown in randomly whenever the haemoglobin result comes back low. Traditional methods of trauma resuscitation were "unbalanced". Achieve this whole-blood-like ratio within the first 6 hours of resuscitation.Reverse fibrinolysis associated with massive blood loss. 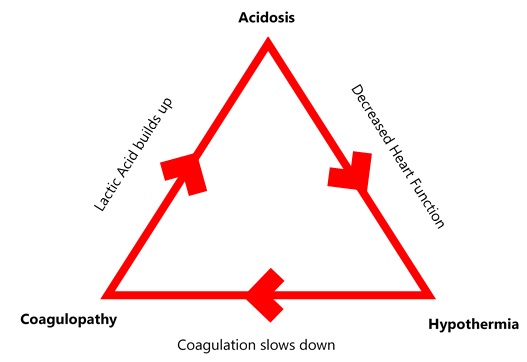
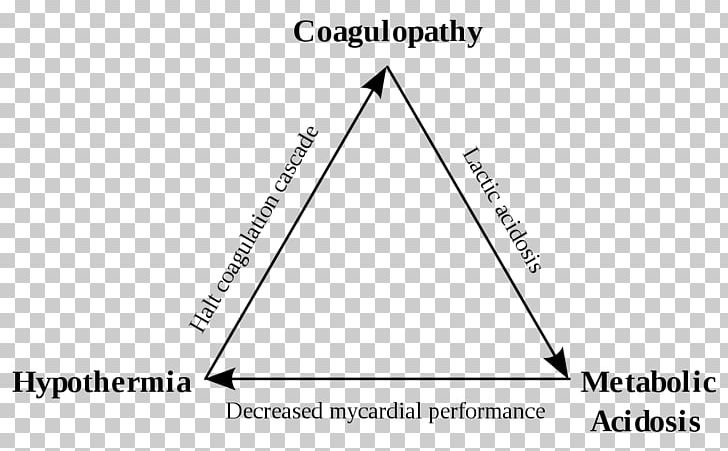
Use blood components in a proportion which resembles whole blood.Resuscitation with a balanced combination of blood products, which in combination resemble the composition of whole blood, aiming to avoid dilutional coagulopathy.Rapid correction of haemostasis-impairing factors, such as hypothermia hypocalcemia and acidosis.At the same time, it is important to limit the total amount of infused crystalloid, so as to avoid excessive organ oedema. The Critical Bleeding/Massive Tranfusion Module from the National Blood Authority is the definitive resource for the "official position". The main message is the management of the "lethal triad" - correction of hypothermia, acidosis and coagulopathy. For a good long-form review, one may turn either to Heiko Lier et al (2008) or to this 2016 dissertation by Lana Castellucci. There is a lot written on this topic- much more than an exhausted exam candidate can be expected to internalise. There is no high-quality evidence to support the use of any specific plasma : platelets : red cell ratio, but the PROPPR trial did find a statistically significant mortality improvement within the first 24 hours with the 1:1:1 ratio.These goals (including the balanced transfusion ratio) should be achieved within the first 6 hours of resuscitation.A key feature is the use of "balanced" blood product transfusion (1:1:1) of platelets, plasma and PRBCs.The goals of haemostatic resuscitation are to correct acidosis, hypothermia and coagulopathy in trauma.This article explores the pathogenesis and treatment of acidosis, hypothermia, and coagulopathy as it applies to the exsanguinating trauma patient. Critical care nurses must underetand this triad, because it forms the basis and underlying logic on which the damage control philosophy has been built. The “new” golden hour may well be the time in the operating room before the patient reaches the physiologic limit, defined as the onset of the triad: hypothermia, acidosis and coagulopathy. As the shift in care of patients in extremis has continued to move from the street to the emergency department and beyond, the focus of trauma resuscitation has shifted to the operating room and ultlmately to the intensive care unit. The concept of the “golden hour” has translated into unprecedented speed and efficiency of trauma resuscitation with the ultimate goal of short injury-to-incision times. With the organization of trauma systems, the development of trauma centers, the application of standardized methods of resuscitation, and improvements in modern blood banking techniques, the ability to aggressively resuscitate patients in extremis has evolved.
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
